Archive for the ‘Rabies’ Category
Rabies in a Dog: From Egypt to Connecticut (2017)
Friday, December 21st, 2018Hercules Y, Bryant NJ, Wallace RM, et al. Rabies in a Dog Imported from Egypt — Connecticut, 2017. MMWR Morb Mortal Wkly Rep 2018;67:1388–1391. DOI: http://dx.doi.org/10.15585/mmwr.mm6750a3.
“……Since 2007, three cases of canine rabies virus variant were reported in dogs imported into the United States, one each from India (2007), Iraq (2008), and Egypt (2015) (1–3). On December 20, 2017, a dog imported into the United States from Egypt was identified with rabies, representing the second case from Egypt in 3 years. An Egyptian-based animal rescue organization delivered four dogs from Cairo, Egypt, to a flight parent (a person solicited through social media, often not affiliated with the rescue organization, and usually compensated with an airline ticket), who transported the dogs to the United States. The flight parent arrived at John F. Kennedy International Airport (JFK) in New York City and, via transporters (persons who shuttle dogs from one state to another), transferred the dogs to foster families; the dogs ultimately were adopted in three states. The Connecticut Department of Public Health Laboratory (CDPHL) confirmed the presence of a canine rabies virus variant in one of the dogs, a male aged 6 months that was adopted by a Connecticut family. An investigation revealed the possibility of falsified rabies vaccination documentation presented on entry at JFK, allowing the unvaccinated dog entry to the United States. This report highlights the continuing risk posed by the importation of dogs inadequately vaccinated against rabies from high-risk countries and the difficulties in verifying any imported dog’s health status and rabies vaccination history.….”
Asia: The dog meat industry & rabies
Thursday, October 4th, 2018‘……The Centres for Disease Control and Prevention of the United States said: “There are reports that dog-meat markets have a higher rate of rabies than the general dog population, as people often sell dogs to the markets when they act sick; some of these sick dogs have rabies.
“Furthermore, there are at least three published reports of humans acquiring rabies from activities associated with the dog meat market, emphasizing that the risk is very real.”…….’
The Philippines: 8 people died of dog rabies in Western Visayas from January until August, 2018 and 4 of the deaths recorded were children below 15 years of age.
Monday, October 1st, 2018Yangon General Hospital, Myanmar: Eighteen people died from rabies in the first eight months of this year
Tuesday, September 4th, 2018- That number could increase if other hospitals across the country are included in the total.
- Last year, the hospital treated and vaccinated 16,274 people for dog bites. Of those patients, 32 died from rabies.
WHO, the UN Food and Agriculture Organization (FAO), the World Organisation for Animal Health (OIE), and the Global Alliance for Rabies Control (GARC) are joining forces to support countries as they seek to accelerate their actions towards the elimination of dog-mediated rabies by 2030.
Thursday, June 28th, 2018“……The Global Strategic Plan set three objectives for affected countries, development partners, and key stakeholders: (1) to effectively use vaccines, medicines, tools, and technologies that will stop dog rabies transmission and reduce the risk of human rabies deaths; (2) to generate evidence-based guidance and high-quality data to measure impact and inform policy decisions; and (3) to harness multistakeholder engagement to sustain commitment and resources...…”
PHILIPPINES: Twelve residents who ate dog meat are under observation for rabies
Friday, April 6th, 2018
“….The residents….ate the dog meat which was cooked by the owner of the dog, who also slaughtered the animal himself…..
The owner reportedly did this after the dog bit him.
After 15 days, the owner passed away……”
Rabies Deaths Among Pregnant and Breastfeeding Women — Vietnam
Wednesday, April 4th, 2018Nguyen HT, Tran CH, Dang AD, et al. Rabies Vaccine Hesitancy and Deaths Among Pregnant and Breastfeeding Women — Vietnam, 2015–2016. MMWR Morb Mortal Wkly Rep 2018;67:250–252. DOI: http://dx.doi.org/10.15585/mmwr.mm6708a4.
“…..Despite widespread availability of PEP in Vietnam, in 2015 the Ministry of Health (MoH) received reports of pregnant and breastfeeding women with clinically diagnosed rabies. MoH investigated factors associated with these rabies cases. MoH found that, during 2015–2016, among 169 cases reported in Vietnam, two probable cases of rabies were reported in breastfeeding mothers and four in pregnant women, all of whom had been bitten by dogs. All six patients died. Three of the four pregnant women had cesarean deliveries. One of the three newborns died from complications believed to be unrelated to rabies; the fourth pregnant woman contracted rabies too early in pregnancy for the fetus to be viable. Two of the patients sought care from a medical provider or traditional healer; however, none sought PEP after being bitten. In each case, families reported the patient’s fear of risk to the fetus or breastfed child as the primary barrier to receiving PEP. These findings highlight the need for public health messaging about the safety and effectiveness of PEP in preventing rabies among all persons with exposures, including pregnant and breastfeeding women.……”
* Family reported that the dog appeared normal at the time of exposure. No information was available regarding the status of the dog after 10 days.
† Patients could have multiple symptoms.
Stray dog situation in Thailand out of control & thus, the risk of rabies grows
Tuesday, March 27th, 2018“…..According to the last nationwide survey in 2014 there are around eight and a half million dogs in Thailand. Seven hundred thousand of those are considered to be strays with a round half of that number being females who produce up to ten puppies a year. This figure means that the stray canine population could increase by up to 3.4 million dogs a year.
Stray dogs as well as being unclean and causing noise pollution can also spread diseases such as rabies. 90% of the animals found with rabies in Thailand are dogs and 60% of rabid dogs are strays…..”
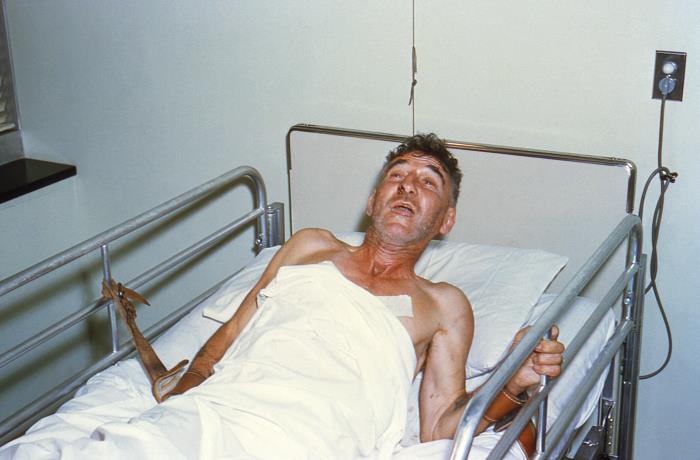
CDC: This patient presented with early, though progressive symptoms due to what was confirmed as rabies virus.
Latest research: Rabies in bats and carnivores, and implications for spillover to humans
Thursday, November 9th, 2017Comparative pathogenesis of rabies in bats and carnivores, and implications for spillover to humans
Published online: October 31, 2017
Lineke Begeman, Corine GeurtsvanKessel, Stefan Finke, Conrad M Freuling, Marion Koopmans, Thomas Müller, Tom J H Ruigrok, Thijs Kuiken
The Lancet Infectious Diseases
http://www.thelancet.com/journals/laninf/article/PIIS1473-3099(17)30574-1/fulltext