Archive for April, 2019
Konzo, a food-borne illness that paralyzes the legs and back, has been raging in Feshi territory in southwestern Democratic Republic of the Congo (DRC)’s Kwango province for several months.
Sunday, April 28th, 2019“……Le konzo est une maladie qui attaque les membres inférieurs et la colonne vertébrale, provoquant une déformation physique déplorable et souvent irréversible. Cette maladie est provoquée par la consommation d’une variété de manioc très amer qui devait normalement rester trempé dans l’eau au moins pendant quatre jours pour éliminer le cyanure avant d’être consommé...…”
Cassava, konzo, and neurotoxicity
Breaking news: A man walked into the Chabad synagogue in Poway, CA and started shooting causing at least 4 casualties with 1 confirmed death
Saturday, April 27th, 20194/27/1865: The steamboat Sultana explodes on the Mississippi River near Memphis, killing 1,700 passengers and Union soldiers.
Saturday, April 27th, 2019Lassa and Crimean-Congo Hemorrhagic Fever in Mali
Saturday, April 27th, 2019Baumann, J., Knüpfer, M., Ouedraogo, J., Traoré, B. Y., Heitzer, A., Kané, B….Wölfel, R. (2019). Lassa and Crimean-Congo Hemorrhagic Fever Viruses, Mali. Emerging Infectious Diseases, 25(5), 999-1002.
“…..We detected LASV RNA in blood samples from 2 patients, a 5-year-old boy and a 13-year-old girl. Both children were treated for episodes of high fever during September–October 2016 at the Hôpital du Mali……..Using reverse transcription quantitative PCR, we detected acute CCHFV infection in 2 patients hospitalized at Hospital Gabriel Touré in April 2017, a 1-year-old boy (cycle threshold 32.74) and a 2-year-old boy (cycle threshold 36.95)…….”
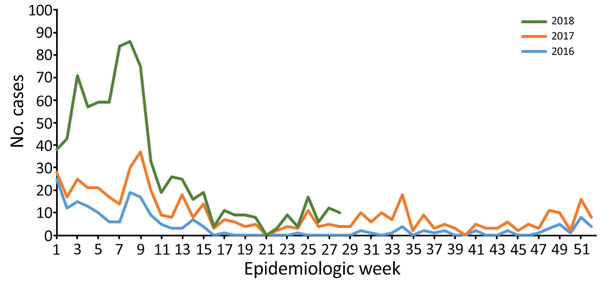
2018: Lassa Fever in Nigeria
Saturday, April 27th, 2019| Ilori EA, Frank C, Dan-Nwafor CC, Ipadeola O, Krings A, Ukponu W, et al. Increase in Lassa Fever Cases in Nigeria, January–March 2018. Emerg Infect Dis. 2019;25(5):1026-1027.
Weekly trends of confirmed Lassa fever cases, Nigeria, 2016–2018.
“……A total of 107 laboratory-confirmed cases were reported during the first 12 weeks of 2017 and 394 during the same period in 2018. Among confirmed and probable cases, 50 deaths were reported during the peak season in 2017 and 104 in 2018. ……” |
Severe Fever with Thrombocytopenia Syndrome in Vietnam
Saturday, April 27th, 2019Tran X, Yun Y, Van An L, Kim S, Thao NT, Man PC, et al. Endemic Severe Fever with Thrombocytopenia Syndrome, Vietnam. Emerg Infect Dis. 2019;25(5):1029-1031. https://dx.doi.org/10.3201/eid2505.181463
“…..Severe fever with thrombocytopenia syndrome virus (SFTSV) is a tickborne virus (genus Phlebovirus, family Phenuiviridae) that can cause a mild to severe febrile illness similar to hemorrhagic fever…..
On October 29, 2017, a 29-year-old woman (Hue 06-Vietnam-10-2017) was hospitalized at Hue University Hospital because of headache, vomiting, and gum bleeding. She lived in Hue City and was unaware of having received an insect bite. Her temperature was 38°C, and blood tests showed leukopenia (leukocyte count 1,900 cells/μL [reference 4,000–10,000 cells/μL]), thrombocytopenia (platelet count 125 × 103/μL [reference 150–450 × 103/μL]), and a low hematocrit level (34.3% [reference 36%–44%]). The patient fully recovered without other complications after 5 days.
On November 2, 2017, a 27-year-old man (Hue 13-Vietnam-11-2017) was hospitalized at Hue University Hospital because of headache and fatigue. He had had dengue fever at 8 years of age. Blood tests showed thrombocytopenia (platelet count 14 × 103/μL), normal leukocyte count (7,410 cells/μL), mildly elevated aspartate aminotransferase (84 IU/L [reference 8–38 IU/L]), elevated alanine aminotransferase (98 IU/L [reference 4–44 IU/L]), and mildly elevated hematocrit (47.6% [reference 36%–44%]). He fully recovered without other complications after 7 days…….”
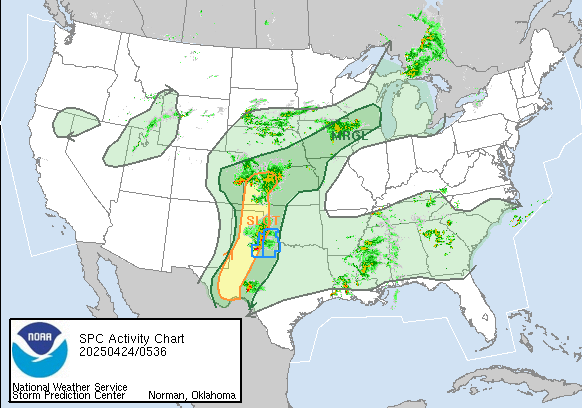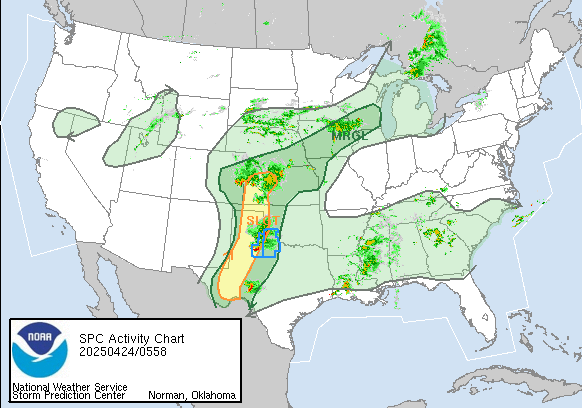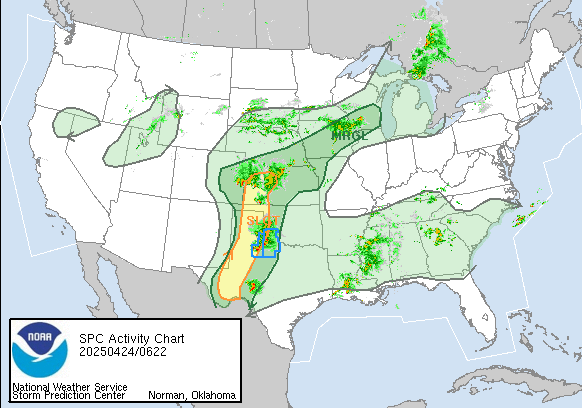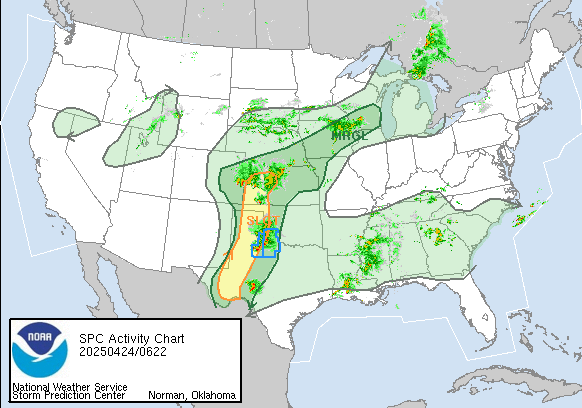
At least one earthquake happens every three minutes across Southern California.
Saturday, April 27th, 2019“…….When they started their research, the earthquake catalog for the region of Southern California they studied listed 181,000 temblors recorded between 2008 and 2017. After wading through the data and scanning it through high-power computers, that number was increased to 1.8 million.
The nearly 2 million “new” earthquakes range in magnitude from negative 2.0 to 1.7……”

| Satellite image of southern California showing superposed fault lines (image sources: (1) faults from Jennings, 1994; (2) Landsat image from Jet Propulsion Laboratory of the California Institute of Technology). [Jennings, C.W., 1994, Fault activity map of California and adjacent areas: California Division of Mines and Geology, California Geologic Data Map Series, Map No. 6, scale 1:750,000. ] |
|
|
 |
| Oblique aerial photograph of the trace of a fault on the desert floor of southern California; view looking east at the Coachella Valley trace of the Banning Fault in the northern Coachella Valley. The linear trace on the desert floor occurs where a fault plane that is vertical in the subsurface intersects the land surface. Thus, a cross-sectional view of a fault in a road cut expresses translates into a trace on the ground surface when viewed from above in this photograph. The linear is formed by scarps (topographic expression of fault movement), by vegetation concentrated along the fault trace where ground-water ponds up-slope from the fault, and by sand dunes that form where wind-blown sand is trapped by the vegetation. Photo by J.C. Matti, USGS, December, 1979. |
 |
Diagram illustrating the plate-tectonic setting of southern California (image source: USGS general-interest publication “This dynamic earth: the story of plate tectonics” (Kious and Tilling, 1996). |
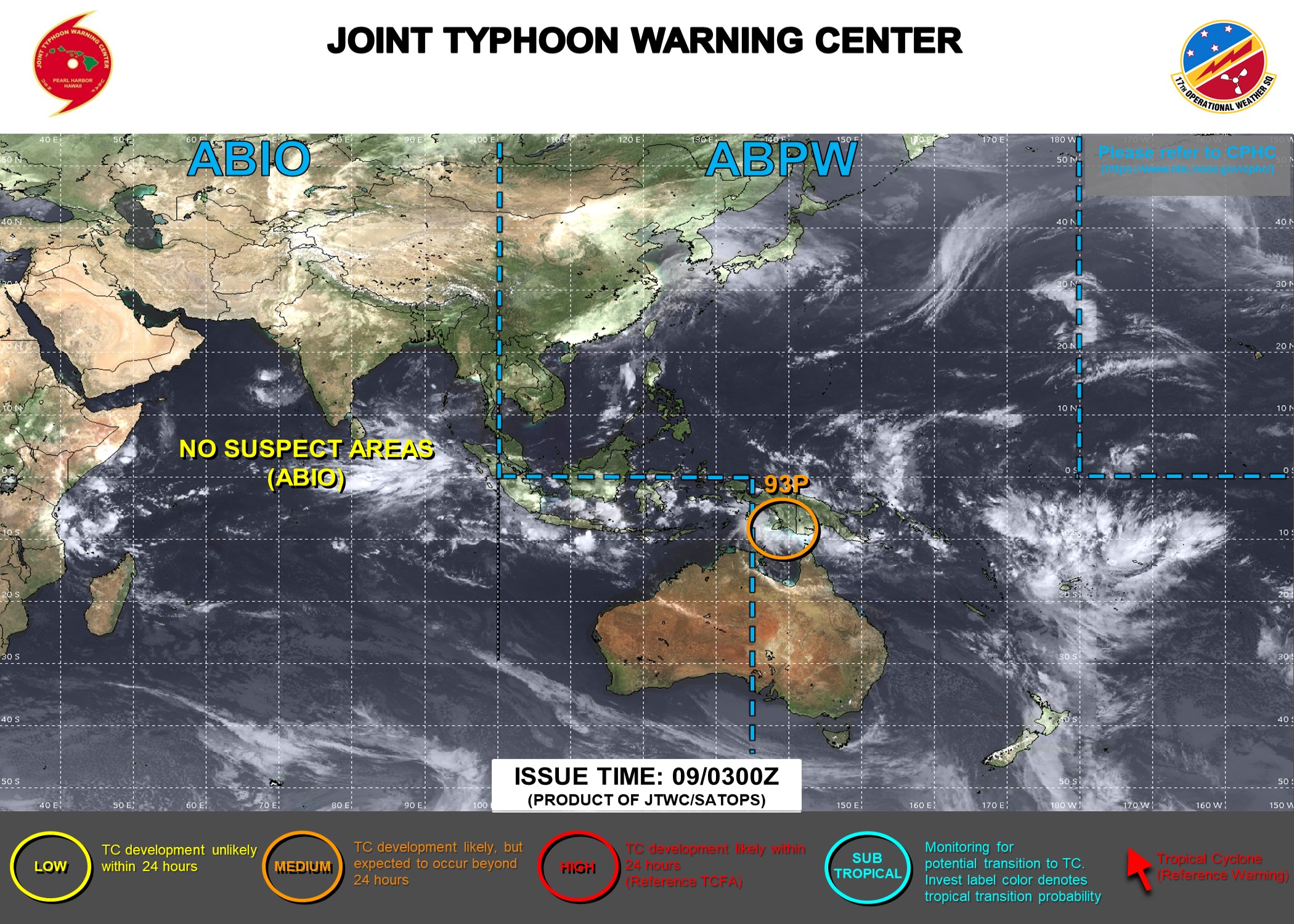
A MERS-CoV outbreak in Wadi ad-Dawasir, Saudi Arabia: Since January, officials have identified 61 cases in the city, of which 14 were in health workers, and 37 were thought to involve healthcare exposure.
Saturday, April 27th, 2019Middle East respiratory syndrome coronavirus (MERS-CoV) – The Kingdom of Saudi Arabia
From 14 February through 31 March 2019, the National IHR Focal Point of Saudi Arabia reported 22 additional cases of Middle East respiratory syndrome coronavirus (MERS-CoV) infection, including four deaths, associated with the outbreak in Wadi Aldwasir. Of the 22 cases, 19 were reported from Wadi Aldwasir city including two healthcare workers. The remaining three cases, which are epidemiologically linked to the outbreak, were healthcare workers from a hospital in Khamees Mushait city, Asir region.

Since the beginning of this outbreak in January 2019, a total of 61 MERS-CoV cases, with a case fatality ratio of 13.1% (8/61), have been reported in Wadi Aldwasir city. The median age of reported cases was 46 years (range 16 to 85 years). Of the 61 cases, 65% (n=46) were male, and 23% (n = 14) were health care workers. Investigations into the source of infection of the 61 cases found that 37 were health-care acquired infections, 14 were primary cases presumed to be infected from contact with dromedary camels and the remaining (10) infections occurred among close contacts outside of health care settings. As previously reported1, two human to human transmission amplification events took place at a hospital during this outbreak (one amplification event in the emergency department, and one amplification event in a cardiac intensive care unit; Figure 1).
The link below provides details of the 22 reported cases:
From 2012 through 31 March 2019, a total of 2399 laboratory-confirmed cases of MERS-CoV and 827 associated deaths were reported globally to WHO under the International Health Regulations (IHR). The associated deaths reported to WHO were identified through follow-up with affected member states.
Public Health Response
As reported previously, the Saudi Arabian Ministry of Health (MoH) has conducted and completed a full-scale investigation of the MERS outbreak in Wadi Aldwasir including identification of all household and healthcare worker contacts of confirmed patients in all of the hospitals affected.
As of 31 March 2019, a total of 380 contacts have been identified, including 260 household contacts and 120 healthcare worker contacts. All identified contacts were monitored for 14 days from the last date of exposure as per WHO and national guidelines for MERS. All secondary cases have been reported to WHO.
Currently, all the listed contacts have been tested for MERS-CoV infection by reverse transcription polymerase chain reaction (RT-PCR) at least once and many contacts of known patients have been tested repeatedly. All secondary cases of MERS-CoV infection have been reported to WHO. The last case from Wadi Aldwasir was reported on 12 March 2019.
Within the affected health care facilities, infection prevention and control measures have been enhanced including intensive mandatory on-the-job training on infection control measures for all healthcare workers in emergency room and intensive care unit. Disinfection has been carried out in the emergency room and ICU of hospital A, which is fully operational and additional staff were mobilized to support infection control activities. Respiratory triage has been enforced in all healthcare facilities in the Riyadh region.
The MoH media department launched an awareness campaign targeting Wadi Aldawasir city with special focus on camel owners and camel related activities.
The Ministry of Agriculture is testing dromedaries in Wadi Aldwasir city and initial results have identified several PCR positive dromedaries in the city. Positive camels have been removed from the market and movement in and out of the camel market has been restricted. Camels owned by confirmed human cases were quarantined regardless of testing results. Full genome sequencing of available human and dromedary specimens have been conducted. Laboratory findings of camel testing by the Ministry of Agriculture have been reported to the World Organization for Animal Health (OIE).
WHO risk assessment
Infection with MERS-CoV can cause severe disease resulting in high morbidity and mortality. Humans are infected with MERS-CoV from direct or indirect contact with infected dromedary camels or by transmission between humans. So far, the observed non-sustained human-to-human transmission has occurred mainly in health care settings.
The notification of these additional cases does not change WHO’s overall risk assessment of MERS. WHO expects that additional cases of MERS will be reported from the Middle East, and that cases will continue to be exported to other countries by individuals who might acquire the infection after exposure to dromedary camels, dromedary camel animal products (for example, consumption of camel’s raw milk), or humans (for example, in a health care setting or household contacts).
WHO continues to monitor the epidemiological situation and conducts risk assessment based on the latest available information. Results of the completed epidemiological investigation, as well as full genome sequencing of available dromedary and human specimens are being used by Ministry of Health officials to further evaluate the zoonotic and human-to-human transmission that has occurred in Wadi Aldwasir outbreak.
WHO advice
Based on the current situation and available information, WHO encourages all Member States to continue their surveillance for acute respiratory infections and to carefully review any unusual patterns.
Infection prevention and control (IPC) measures are critical to prevent the possible spread of MERS-CoV in health care facilities. It is not always possible to identify patients with MERS-CoV infection early because like other respiratory infections, the early symptoms of MERS are non-specific. Therefore, healthcare workers should always apply standard precautions consistently with all patients, regardless of their diagnosis. Droplet precautions should be added to the standard precautions when providing care to patients with symptoms of acute respiratory infection; contact precautions and eye protection should be added when caring for probable or confirmed cases of MERS; airborne precautions should be applied when performing aerosol generating procedures.
Early identification, case management and isolation, together with appropriate infection prevention and control measures can prevent human-to-human transmission of MERS-CoV.
WHO recommends that comprehensive identification, follow up and testing of all contacts of MERS patients be conducted, if feasible, regardless of the development of symptoms since approximately 20% of all reported MERS cases have been reported as mild or asymptomatic. The role of asymptomatic MERS-CoV infection in transmission is not well understood. However, reports of transmission from an asymptomatic MERS patient to another individual have been documented.
MERS causes more severe disease in people with underlying chronic medical conditions such as diabetes mellitus, renal failure, chronic lung disease, and compromised immune systems. Therefore, people with these underlying medical conditions should avoid close unprotected contact with animals, particularly dromedary camels, when visiting farms, markets, or barn areas where the virus is known to be potentially circulating. General hygiene measures, such as regular hand washing before and after touching animals and avoiding contact with sick animals, should be adhered to.
Food hygiene practices should be observed. People should avoid drinking camel’s raw milk or camel urine or eating camel meat that has not been properly cooked.
WHO does not advise special screening at points of entry with regard to this event nor does it currently recommend the application of any travel or trade restrictions.