Archive for the ‘Rabies’ Category
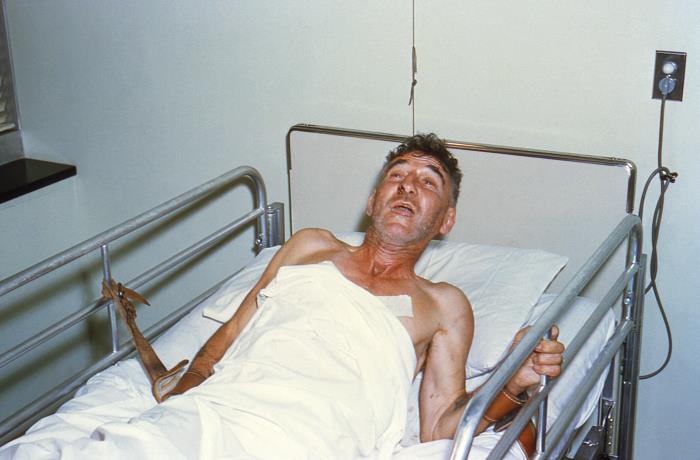
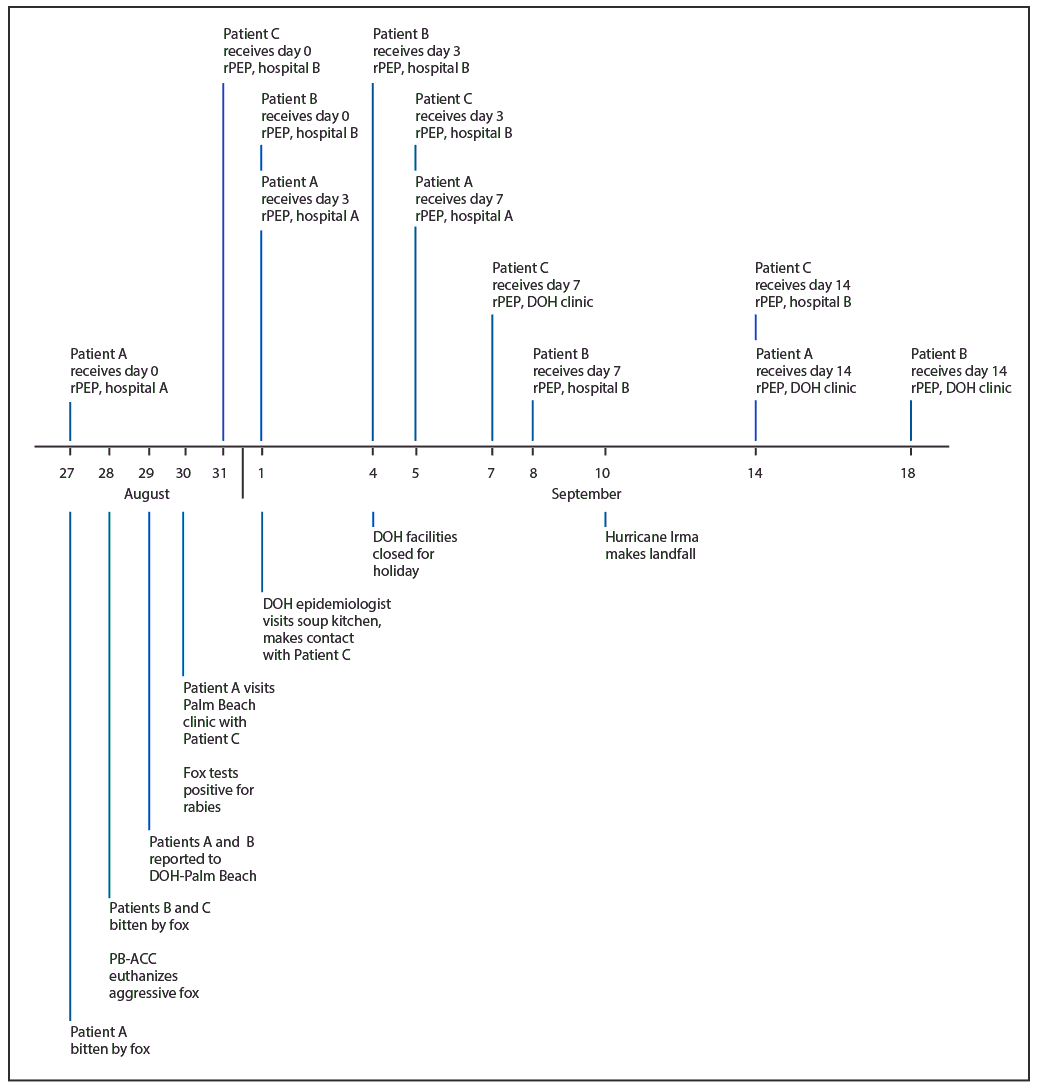
Challenges to Completing Rabies Postexposure Prophylaxis After Hurricane Irma
Tuesday, September 17th, 2019O’Sullivan B, Burke R, Bassaline D. Notes from the Field: Rabies Exposures from Fox Bites and Challenges to Completing Postexposure Prophylaxis After Hurricane Irma — Palm Beach County, Florida, August–September 2017. MMWR Morb Mortal Wkly Rep 2019;68:795–797. DOI: http://dx.doi.org/10.15585/mmwr.mm6836a4external icon
WHO: Eliminate human rabies by 2030
Tuesday, August 13th, 2019
United Against Rabies launches global plan to achieve zero rabies human deaths
18 June 2018 | Paris | Geneva | Rome | Manhattan (KS) −− Investing approximately US$ 50 million between now and 2030 can support the elimination of dog-mediated human rabies. A strategic plan that provides a phased, all-inclusive, intersectoral approach to eliminate human deaths from rabies has just been launched by United Against Rabies, a collaboration of four partners: the World Health Organization (WHO), the Food and Agriculture Organization of the United Nations (FAO), the World Organisation for Animal Health (OIE) and the Global Alliance for Rabies Control (GARC).
Zero by 30: the global strategic plan to end human deaths from dog-mediated rabies by 2030 was prepared following a global call in 2015 to “end human rabies deaths by 2030”.
The plan, finalized in consultation with relevant global, regional and country stakeholders, builds on the current international momentum to eliminate rabies.
In alignment with the United Nations Sustainable Development Goals and health for all, Zero by 30 advocates for investment to strengthen human and animal health systems and save lives.
A summary of the plan was made available on the last World Rabies Day (28 September).
The plan provides a coordinated response to rabies prevention, integrated with strengthening of human and veterinary health systems, in order to reach the world’s most underserved populations by engaging, empowering and enabling all countries to lead and strengthen elimination efforts.
In up to 99% of cases, domestic dogs are responsible for transmission of rabies virus to humans, which occurs mostly through bites or scratches, usually via saliva. Rabies is 100% vaccine-preventable, yet the disease kills almost 59 000 people every year – or one person every nine minutes, 40% of whom are children living in Asia and Africa.
The world has the knowledge, technology and vaccines that are needed to eliminate rabies. The plan supported by the four partners aims to:
- prevent and respond to dog-transmitted rabies by improving awareness and education, reducing human rabies risk through expanded dog vaccinations, and improving access to healthcare, medicines and vaccines for populations at risk;
- generate and measure impact by implementing proven effective guidance for rabies control, and encouraging the use of innovative surveillance technologies to monitor progress towards Zero by 30; and
- demonstrate the impact of the United Against Rabies collaboration in national, regional and global rabies elimination programmes, in order to ensure continued stakeholder engagement at all levels and sustained financing to achieve Zero by 30.
Rabies: Zero by 30
Saturday, August 10th, 2019Overview

Why eliminate rabies?
An estimated 59 000 people die from rabies each year. That’s one person every nine minutes of every day, 40% of whom are children living in Asia and Africa. As dog bites cause almost all human cases, we can prevent rabies deaths by increasing awareness, vaccinating dogs to prevent the disease at its source and administering life-saving treatment after people have been bitten. We have the vaccines, medicines, tools and technologies to prevent people from dying from dog-mediated rabies. For a relatively low cost it is possible to break the disease cycle and save lives.
A country’s health system benefits from the capacity-building required for rabies surveillance. This core activity strengthens the health system by improving the mechanisms for surveillance of other disease and expanding access to health care. Minimizing duplication and improving efficiencies by pooling resources and developing strong health service networks saves money and makes the most of resources. Countries can maximize the impact of each dollar invested.
Investing in rabies elimination saves lives and strengthens both human and veterinary health systems. A collaborative response, through rabies programmes, contributes to disease prevention and preparedness. This means integrated rabies elimination is a model for One Health collaboration.
In the past, the global response has been fragmented and uncoordinated. We need to break the status quo and come together with a combined will, an achievable goal and a common plan. That combined will was evident in 2015, and the resulting global call to action made it clear that now is the time to act.
A call for action
In 2015, the world called for action by setting a goal of zero human dog-mediated rabies deaths by 2030, worldwide. Now, for the first time, four organizations – the World Health Organizaton (WHO), the World Organisation for Animal Health (OIE), the Food and Agriculture Organization of the United Nations (FAO) and the Global Alliance for Rabies Control (GARC) – have joined forces, as the United Against Rabies collaboration, and are determined to reach this goal.
The United Against Rabies collaboration leverages existing tools and expertise in a coordinated way to empower, engage and enable countries to save human lives from this preventable disease. The global strategic plan puts countries at the centre with renewed international support to act.This country-centric engagement will be flexible and consider different contexts and capacities. Countries will lead efforts, driving the changes needed to reach Zero by 30, empowered by the United Against Rabies collaboration, as they build sustainable institutional capacity and end human deaths from dog-mediated rabies.

“…..Worldwide, about 59,000 people a year die from rabies, most in Africa and Asia, 99 percent of them because they were bitten by a rabid dog…..”
Wednesday, August 7th, 2019“…….Mission Rabies, which is part of Worldwide Veterinary Service and supported partly by Dogs Trust Worldwide, both nonprofits, has targeted Goa as a place to demonstrate the viability of its program to stop the spread of canine rabies. It spends about $300,000 a year and has vaccinated 100,000 dogs a year since 2017, about 50,000 a year before that. Deaths of people from rabies in Goa fell to zero last year from 15 in 2014, when the campaign started. There are none so far in 2019. ……”
CDC
Pakistan is short of at least 800,000 doses of rabies vaccine
Monday, July 8th, 2019“…….Health officials in the province of Sindh said doctors in the city of Karachi were seeing as many as 150 dog bite cases a day and 11 people have died so far this year……
The shortage was disclosed amid similar shortfalls in neighbouring India…….
Rabies kills around 60,000 people a year and is present in more than 150 countries, but is considered a neglected disease mainly affecting the rural poor…..”
A 24-year-old Norwegian woman died this week of rabies, after she was bitten by a puppy she rescued while on a Philippine vacation
Sunday, May 12th, 2019“……At least 59 000 people worldwide die each year worldwide from the animal-borne disease, according to the World Health Organization (WHO). More than 99% of victims are concentrated in Asia, Africa and South America…….”
Thailand: First case of human rabies this year
Monday, April 29th, 2019“……A 32 year old man in Surin province has become the first person to die of Rabies this year.
The Disease Control Department director-general Dr Suwannachai Wattanayingcharoenchai says the man who was bitten by a stray dog last November but never sought an anti-Rabies vaccination.
The man developed fever and had difficulty swallowing….”

WHO warns against a counterfeit anti-rabies vaccine now circulating in the Philippines.
Sunday, February 3rd, 2019“….The WHO said that “two falsified vaccines have so far been discovered.” It said that Verorab vaccines with batch number NIE35 and H1833 are counterfeit.….”
Destined to die – the price for contact with a puppy in India.
Friday, January 4th, 2019“…..The patient had been on a seven-week-long yoga retreat in India just weeks before. “Tour members confirmed that the patient was bitten by a puppy outside her hotel in Rishikesh, India, and that the wound was washed with water, but no further treatment was administered,” Virginia’s chief veterinarian, Dr. Julia Murphy…..the patient’s husband reported that she had been bitten on the right hand by a puppy approximately six weeks before symptom onset while touring in India…….”
A five-year-old boy died Saturday in a Santo Domingo hospital from rabies, the fourth such case of the year in the Dominican Republic
Wednesday, January 2nd, 2019“…..The boy was bitten by a dog on November 19….and ten days later he was subjected to an antirabies vaccination scheme, receiving four doses…..”
CDC: Vaccination after an exposure
“….Anyone who has been bitten by an animal, or who otherwise may have been exposed to rabies, should clean the wound and see a doctor immediately. The doctor will determine if they need to be vaccinated.
A person who is exposed and has never been vaccinated against rabies should get 4 doses of rabies vaccine – one dose right away, and additional doses on the 3rd, 7th, and 14th days. They should also get another shot called Rabies Immune Globulin at the same time as the first dose…..”