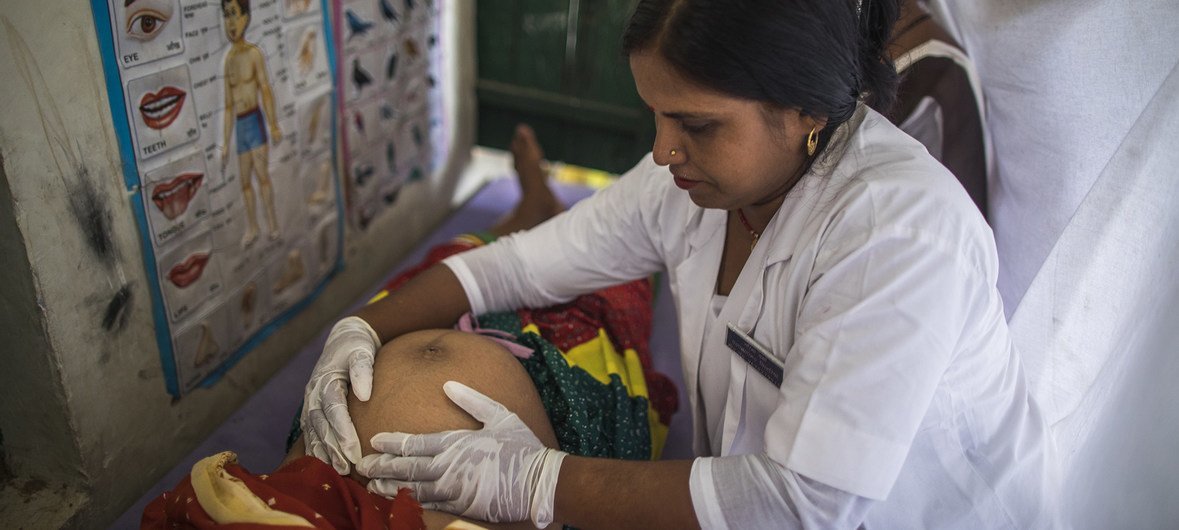
Health services must integrate a stronger focus on ensuring optimum nutrition at each stage of a person’s life, according to a new report released by the World Health Organization (WHO). It is estimated that the right investment in nutrition could save 3.7 million lives by 2025[1].
“In order to provide quality health services and achieve Universal Health Coverage, nutrition should be positioned as one of the cornerstones of essential health packages,” said Dr Naoko Yamamoto, Assistant Director-General at WHO. “We also need better food environments which allow all people to consume healthy diets.”
Essential health packages in all settings need to contain robust nutrition components but countries will need to decide which interventions best support their national health policies, strategies and plans.
Key interventions include: providing iron and folic acid supplements as part of antenatal care; delaying umbilical cord clamping to ensure babies receive important nutrients they need after birth; promoting, protecting and supporting breastfeeding; providing advice on diet such as limiting the intake of free sugars[2] in adults and children and limiting salt intake to reduce the risk of heart disease and stroke.
Investment in nutrition actions will help countries get closer to their goal of achieving universal health coverage and the Sustainable Development Goals. It can also help the economy, with every US$1 spent by donors on basic nutrition programmes returning US$ 16 to the local economy[3].
The world has made progress in nutrition but major challenges still exist. There has been a global decline in stunting (low height-for-age ratio): between 1990 and 2018, the prevalence of stunting in children aged under 5 years declined from 39.2% to 21.9%, or from 252.5 million to 149.0 million children, though progress has been much slower in Africa and South-East Asia.
Obesity, however, is on the rise. The prevalence of children considered overweight rose from 4.8% to 5.9% between 1990 and 2018, an increase of over 9 million children. Adult overweight and obesity are also rising in nearly every region and country, with 1.3 billion people overweight in 2016, of which 650 million (13% of the world’s population) are obese.
Obesity is a major risk factor for diabetes; cardiovascular diseases (mainly heart disease and stroke); musculoskeletal disorders (especially osteoarthritis – a highly disabling degenerative disease of the joints); and some cancers (including endometrial, breast, ovarian, prostate, liver, gallbladder, kidney, and colon).
An increased focus on nutrition by the health services is key to addressing both aspects of the “double-burden” of malnutrition. The Essential Nutrition Actions publication is a compilation of nutrition actions to address this “double burden” of underweight and overweight and provide a tool for countries to integrate nutrition interventions into their national health and development policies.
[1]World Bank: Source: Shekar M, Kakietek J, D’Alimonte M, Sullivan L , Walters D, Rogers H, Dayton Eberwein J, Soe-Lin S, Hecht R. Investing in nutrition. The foundation for development. An investment framework to reach the Global Nutrition Targets. World Bank, Results for Development, Bill and Melinda Gates Foundation, CIFF,1000 days. http://documents.worldbank.org/curated/en/963161467989517289/pdf/104865-REVISED-Investing-in-Nutrition-FINAL.pdf
[2]Free sugars include monosaccharides and disaccharides added to foods and beverages by the manufacturer, cook or consumer, and sugars naturally present in honey, syrups, fruit juices and fruit juice concentrates
[3]Development Initiatives. Global Nutrition Report 2017: Nourishing the SDGs. Bristol, UK: Development Initiatives, 2017