Archive for May, 2017
A Minneapolis-area measles outbreak that has been fueled by low vaccination rates in Somali-Americans grew to 44
Sunday, May 7th, 2017Minnesota Department of Health
Measles (Rubeola)
Updated 5/5/17
Confirmed cases as of May 5, 2017: 44
(Updated Monday-Friday at 1 p.m.)
-
- 44 total cases:
- 41 in Hennepin County
- 2 in Ramsey County
- 1 in Crow Wing County
- 44 total cases:
- Vaccination status:
- 42 confirmed to be unvaccinated
- 2 had 2 doses of MMR
- Age:
- 43 in children ages 0 through 10 years
- 1 case in an adult
- 38 of the cases are Somali Minnesotan
China: New H7N9 avian flu infections late into the season, with 24 cases reported over the past week, including at least one from a province that had never reported one before.
Sunday, May 7th, 2017May 6, 1937: The hydrogen-filled German dirigible Hindenburg burned and crashed in Lakehurst, N.J., killing 36 of the 97 people on board.
Saturday, May 6th, 2017The Migrant Crisis: The countries bordering the Mediterranean Sea—from Algeria to Egypt in North Africa; from Israel to Syria in the Levant; and Turkey, Greece, and Italy in Europe—are facing unprecedented stress.
Saturday, May 6th, 2017Zika virus IgM can persist beyond 12 weeks in a subset of infected people.
Saturday, May 6th, 2017Distributed via the CDC Health Alert Network
May 05, 2017 1130 ET (11:30 AM ET)
CDCHAN-00402
Prolonged IgM Antibody Response in People Infected with Zika Virus: Implications for Interpreting Serologic Testing Results for Pregnant Women
Summary
In July 2016, CDC issued Interim Guidance for Health Care Providers Caring for Pregnant Women with Possible Zika Virus Exposure – United States, July 2016 (https://www.cdc.gov/mmwr/volumes/65/wr/mm6529e1.htm) that includes Zika virus immunoglobulin M (IgM) testing of pregnant women. However, some flavivirus infections can result in prolonged IgM responses (>12 weeks) that make it difficult to determine the timing of infection, especially in testing of asymptomatic people. Emerging epidemiologic and laboratory data indicate that Zika virus IgM can persist beyond 12 weeks in a subset of infected people. Therefore, detection of IgM may not always indicate a recent infection. Although IgM persistence could affect IgM test interpretation for all infected people, it would have the greatest effect on clinical management of pregnant women with a history of living in or traveling to areas with Zika virus transmission. Pregnant women who test positive for IgM antibody may have been infected with Zika virus and developed an IgM response before conception.
For asymptomatic pregnant women with a history of living in or traveling to areas with Zika virus transmission, Zika virus nucleic acid test (NAT) testing at least once per trimester is recommended, in addition to IgM testing as previously recommended. If positive, this may provide a more definitive diagnosis of recent Zika infection. However, a negative NAT does not rule out recent infection because viral ribonucleic acid (RNA) declines over time. Other diagnostic methods, such as NAT testing of amniocentesis specimens or serial ultrasounds, may provide additional information to help determine whether the IgM test results suggest a recent infection. Providers should counsel women on the limitations of all tests. In addition, providers may wish to consider IgM testing as part of pre-conception counseling to establish baseline IgM results before pregnancy; however, preconception negative IgM results might have limited value for women at ongoing risk of Zika infection. NAT testing should be performed for any pregnant woman who becomes symptomatic or who has a sexual partner who tests positive for Zika virus infection.
Recommendations
For asymptomatic pregnant women with possible Zika virus exposure before conception, (particularly women who lived in or traveled to areas with posted CDC Zika Travel Notices https://wwwnc.cdc.gov/travel/page/zika-information), CDC recommends that healthcare providers take these steps:
- Screen pregnant women for risk of Zika exposure and symptoms of Zika. Promptly test pregnant women with NAT if they become symptomatic during their pregnancy or if a sexual partner tests positive for Zika virus infection.
- Conduct NAT testing at least once per trimester, unless a previous test has been positive.*
- Consider NAT testing of amniocentesis specimens if amniocentesis is performed for other reasons.†
- Counsel pregnant women each trimester on the limitations of IgM and NAT testing. For more information about Zika virus testing, see: https://www.cdc.gov/zika/pdfs/living_in.pdf. For more information about counseling before testing, see: https://www.cdc.gov/zika/pdfs/pretestingcounselingscript_livingin.pdf.
- Consider IgM testing to determine baseline Zika virus IgM levels as part of preconception counseling.§ For more information about preconception counseling, see: https://www.cdc.gov/zika/pdfs/preconception-counseling.pdf
Recommendations for testing symptomatic pregnant women, remain unchanged (https://www.cdc.gov/mmwr/volumes/65/wr/mm6529e1.htm). However, if a symptomatic pregnant woman is IgM positive and NAT negative, and lived in or traveled to an area with a posted CDC Zika Travel Notice (https://wwwnc.cdc.gov/travel/page/zika-information), healthcare providers should recognize that the positive IgM result does not necessarily indicate recent infection.
CDC will update clinical management (https://www.cdc.gov/mmwr/volumes/65/wr/mm6529e1.htm) and laboratory testing (https://www.cdc.gov/zika/laboratories/lab-guidance.html) recommendations as new information becomes available.
Background
Some flavivirus infections have been reported to result in prolonged IgM responses that make it difficult to differentiate recent from prior infections in areas with ongoing transmission. For dengue virus, IgM was determined to persist for 6 months (179 days [95% confidence interval, 155 to 215 days]) for primary infections and 4.6 months (139 days [95% confidence interval, 119 to 167 days]) after infection with another flavivirus1. IgM antibodies against West Nile virus, another flavivirus related to Zika virus, have been detected in asymptomatic, infected blood donors for at least three months after they donated blood, and almost half of tested patients with West Nile virus infection had serum IgM antibodies >1 year after infection2,3.
Recent findings suggest that Zika virus infection may also result in IgM persistence that may make it difficult to differentiate prior from recent infections. A recent study in Puerto Rico of symptomatic patients with NAT-confirmed Zika virus infection detected Zika virus IgM in 100% (28/28) of participants at 8 to 15 days after symptom onset, and 87% (52/60) at greater than 60 days after symptom onset4. Unpublished data on the symptomatic patients from this ongoing study show a median time to first negative Zika virus IgM as 4 months (122 days [range 8-210 days]). More data are needed to accurately estimate the proportion of persons who are likely to have Zika IgM persist beyond 12 weeks after infection.
IgM test results can also be difficult to interpret because of cross-reactivity with other flaviviruses, particularly dengue virus, when a person has been previously infected or vaccinated with a related flavivirus. During 2016, Puerto Rico had limited dengue virus transmission and, therefore, people who tested positive for Zika IgM antibody could be assumed to have had recent Zika virus infection. However, if dengue virus transmission were to increase, guidance for interpretation of Zika virus IgM testing results may need to be reconsidered.
NAT testing may be useful in testing pregnant women as an indicator of current infection and increased risk to the fetus. In the same study from Puerto Rico discussed above, viral RNA was detected in 36% (10/28) of participants at 8‒15 days after symptom onset, 21% (27/129) at 16‒30 days after symptom onset, and 4% (3/79) more than 60 days after symptom onset4. A limited number of studies have demonstrated detection of viral nucleic acid in some pregnant women for even longer periods after symptom onset. For example, three of the five pregnant women included in the study from Puerto Rico had detectable RNA at 46 days and one still had detectable RNA at 80 days after symptom onset4. In another case series, some pregnant women had Zika virus RNA detectable up to 107 days after symptom onset5.
For More Information
Update: Interim Guidance for Health Care Providers Caring for Pregnant Women with Possible Zika Virus Exposure – United States, July 2016. MMWR Morb Mortal Wkly Rep. 2016 Jul 25;65(29):739-44. https://www.cdc.gov/mmwr/volumes/65/wr/mm6529e1.htm
Guidance for U.S. Laboratories Testing for Zika Virus Infection. https://www.cdc.gov/zika/laboratories/lab-guidance.html
Update: Interim Guidance for Preconception Counseling and Prevention of Sexual Transmission of Zika Virus for Persons with Possible Zika Virus Exposure – United States, September 2016. MMWR Morb Mortal Wkly Rep. 2016 Oct 7;65(39):1077-1081. https://www.cdc.gov/mmwr/volumes/65/wr/mm6539e1.htm?s_cid=mm6539e1_w
References
- Prince HE, Matud JL. Estimation of dengue virus IgM persistence using regression analysis. Clin Vaccine Immunol 2011;18: 2183-5.
- Roehrig JT, Nash D, Maldin B, et al. Persistence of virus-reactive serum immunoglobulin M antibody in confirmed West Nile virus encephalitis cases. Emerg Infect Dis 2003;9:376-9. http:// dx.doi.org/10.3201/ eid0903.020531
- Busch MP, Kleinman SH, Tobler LH, et al. Virus and antibody dynamics in acute West Nile virus infection. J Infect Dis 2008;198:984-93. http:// dx.doi.org/10.1086/591467
- Paz-Baily G, Rosenberg ES, Doyle K, et al. Persistence of Zika virus in body fluids— Preliminary report. N Engl J Rep 2017. DOI: 10.1056/NEJMoa1613108
- Suy A, Sulleiro E, Rodó C, et al. Prolonged Zika virus viremia during pregnancy. N Engl J Med. 2016;375:2611-2613.
- Reynolds MR, Jones AM, Petersen EE, et al. Vital signs: Update on Zika virus–associated birth defects and evaluation of all U.S. infants with congenital Zika virus exposure — U.S. Zika pregnancy registry, 2016. MMWR Morb Mortal Wkly Rep 2017;66:366-373.
Footnotes
* Birth defects have been reported in a higher proportion of fetuses or infants whose mothers were infected during the first trimester of pregnancy than in later trimesters. In pregnancies with symptom onset or exposure during the first trimester that were limited to those with laboratory-confirmed Zika virus infection, 15% of completed pregnancies had reported birth defects of the type seen with congenital Zika infection6.
† Consideration of amniocentesis should be individualized, because data about its usefulness in diagnosing congenital Zika virus infection are limited. The presence of Zika virus RNA in the amniotic fluid might indicate fetal infection; however, a negative result does not exclude congenital Zika virus infection
§ Preconceptional IgM testing is recommended to establish a baseline IgM level before pregnancy. However, given the limitations of interpreting IgM testing, the results of these tests should not be used to guide decisions about pregnancy timing for women living in areas with ongoing risk of transmission.
The Department of State alerts U.S. citizens to the continued threat of terrorist attacks throughout Europe.
Tuesday, May 2nd, 2017Europe Travel Alert
The Department of State alerts U.S. citizens to the continued threat of terrorist attacks throughout Europe. This Travel Alert expires on September 1, 2017.
Recent, widely-reported incidents in France, Russia, Sweden, and the United Kingdom demonstrate that the Islamic State of Iraq and ash-Sham (ISIS or Da’esh), al-Qa’ida, and their affiliates have the ability to plan and execute terrorist attacks in Europe. While local governments continue counterterrorism operations, the Department nevertheless remains concerned about the potential for future terrorist attacks. U.S. citizens should always be alert to the possibility that terrorist sympathizers or self-radicalized extremists may conduct attacks with little or no warning.
Extremists continue to focus on tourist locations, transportation hubs, markets/shopping malls, and local government facilities as viable targets. In addition, hotels, clubs, restaurants, places of worship, parks, high-profile events, educational institutions, airports, and other soft targets remain priority locations for possible attacks. U.S. citizens should exercise additional vigilance in these and similar locations, in particular during the upcoming summer travel season when large crowds may be common.
Terrorists persist in employing a variety of tactics, including firearms, explosives, using vehicles as ramming devices, and sharp-edged weapons that are difficult to detect prior to an attack.
If you are traveling between countries in Europe, please check the website of the U.S. embassy or consulate in your destination city for any recent security messages. Review security information from local officials, who are responsible for the safety and security of all visitors to their host country. U.S. citizens should also:
- Follow the instructions of local authorities. Monitor media and local information sources and factor updated information into personal travel plans and activities.
- Be prepared for additional security screening and unexpected disruptions.
- Stay in touch with your family members and ensure they know how to reach you in the event of an emergency.
- Have an emergency plan of action ready.
- Register in our Smart Traveler Enrollment Program (STEP).
We continue to work closely with our European partners and allies on the threat from international terrorism. Information is routinely shared between the United States and our key partners to disrupt terrorist plotting, identify and take action against potential operatives, and strengthen our defenses against potential threats.
For further information:
- See the Department of State’s travel website for the Worldwide Caution, Travel Warnings, Travel Alerts, and Country Specific Information.
- Enroll in the Smart Traveler Enrollment Program (STEP) to receive security messages and make it easier to locate you in an emergency.
- Call 1-888-407-4747 toll-free in the United States and Canada or 1-202-501-4444 from other countries from 8:00 a.m. to 8:00 p.m. Eastern Standard Time, Monday through Friday (except U.S. federal holidays).
- Follow us on Twitter and Facebook.
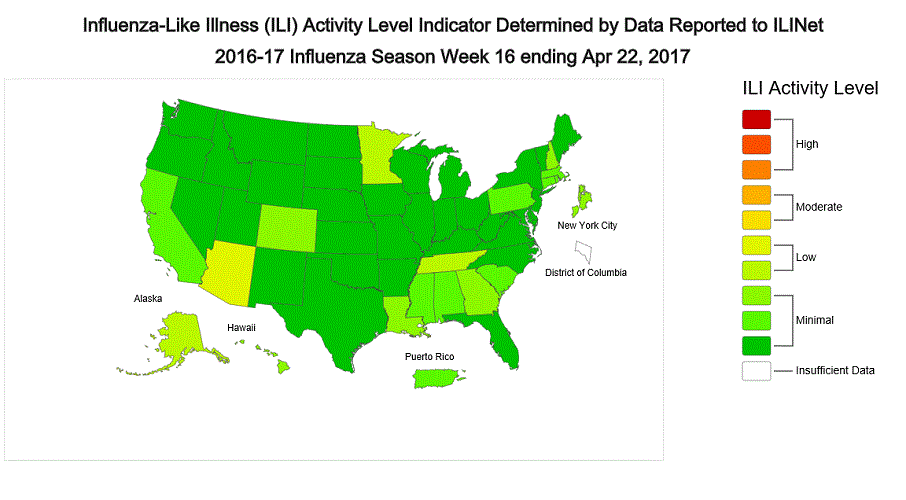
2016-2017 Influenza Season Week 16 ending April 22, 2017
Monday, May 1st, 2017Synopsis:
During week 16 (April 16-22, 2017), influenza activity decreased in the United States.
- Viral Surveillance: The most frequently identified influenza virus type reported by public health laboratories during week 16 was influenza B. The percentage of respiratory specimens testing positive for influenza in clinical laboratories decreased.
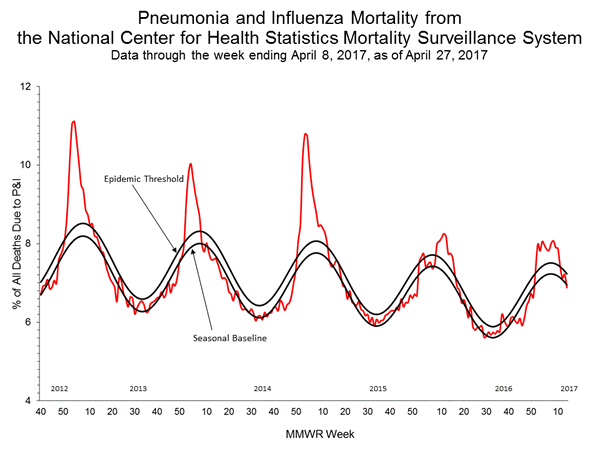
- Pneumonia and Influenza Mortality: The proportion of deaths attributed to pneumonia and influenza (P&I) was below the system-specific epidemic threshold in the National Center for Health Statistics (NCHS) Mortality Surveillance System.
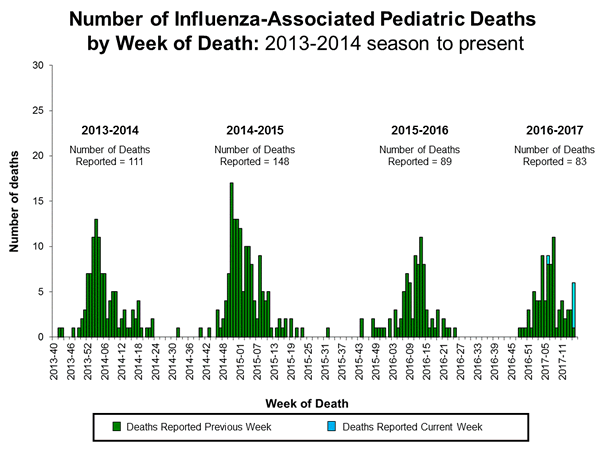
- Influenza-associated Pediatric Deaths:Six influenza-associated pediatric deaths were reported.
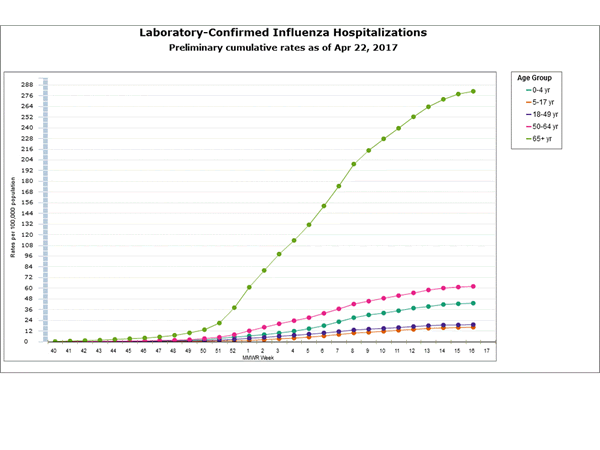
- Influenza-associated Hospitalizations:A cumulative rate for the season of 62.7 laboratory-confirmed influenza-associated hospitalizations per 100,000 population was reported.
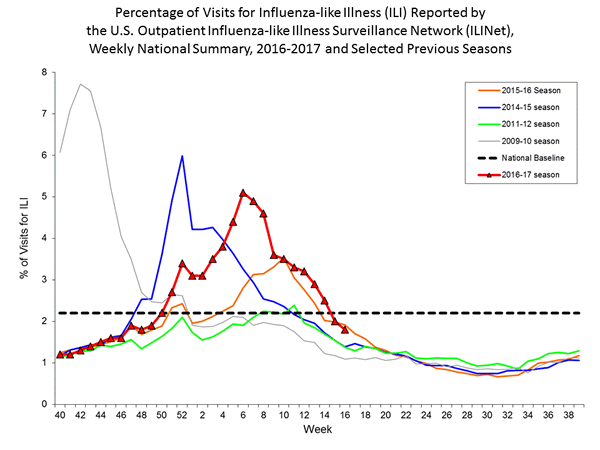
- Outpatient Illness Surveillance: The proportion of outpatient visits for influenza-like illness (ILI) was 1.8%, which is below the national baseline of 2.2%. Two of ten regions reported ILI at or above their region-specific baseline levels. Four states experienced low ILI activity; New York City, Puerto Rico, and 46 states experienced minimal ILI activity; and the District of Columbia had insufficient data.
- Geographic Spread of Influenza: The geographic spread of influenza in seven states was reported as widespread; Guam, Puerto Rico and 11 states reported regional activity; the District of Columbia and 19 states reported local activity; 13 states reported sporadic activity; and the U.S. Virgin Islands reported no activity.