Archive for January, 2019
1/31/1953: North Sea flooding kills more than 1,500 people in the Netherlands, destroys 1 million acres of farmland, wipes out 50,000 buildings and leaves 300,000 homeless
Thursday, January 31st, 2019Bangkok cracks the list of the top 10 cities with the foulest air on the planet.
Thursday, January 31st, 2019“……Bangkok suffers from a toxic amalgam: unchecked industrialization and urbanization, a car-crazy populace and lax regulation. The burning of fallow fields and a dry season with little wind exacerbate the crisis...…”
The Pandemic Response Box
Thursday, January 31st, 2019
About the Pandemic Response Box
The Pandemic Response Box contains 400 diverse drug-like molecules active against bacteria, viruses or fungi.
Request the Pandemic Response Box
The Pandemic Response Box is available free of charge. In return researchers are expected to share data resulting from research on the molecules from the box in the public domain within 2 years of its generation.
Supporting information
All the details related to requesting and conducting research on compounds in the Pandemic Response Box.
Terms & conditions
The agreement between MMV and the requesting institution for the transfer, handling and use of compounds contained in the box.
Australia — again — is in the midst of one of its hottest summers on record.
Thursday, January 31st, 2019WHO Humanitarian Crisis Response Plans: 2018. How successful was it and what about 2019?
Wednesday, January 30th, 2019The WHO Humanitarian Response Plans for 2018 are based on rigorous assessment and analysis of need in 26 countries. The plans include an overview of the situation, WHO’s objectives to address the health aspects of the crisis, and the funds that will be required to do so. They form part of the overall humanitarian response plans developed by partners in the wider humanitarian response.
Reviewing 2017 • In 2017, humanitarian agencies reached more people in need than ever before: tens of millions of them, saving millions of lives; • Donors provided record levels of funding to Humanitarian Response Plans—nearly $13 billion by the end of November; • Humanitarian agencies helped stave off famines in South Sudan, Somalia, north-east Nigeria and Yemen, through effective scale-up and the rapid release of funds by donors; • Agencies stepped up to provide rapid assistance to refugees fleeing violence in Myanmar; and • Mobilized to support countries in the Caribbean to prepare for and respond to successive hurricanes of a ferocity rarely seen before. • Despite conflict and other constraints complicating the provision of assistance, plans were implemented effectively, with costs averaging approximately $230 a year per person for essential needs.
In 2018 • Conflict will continue to be the main driver of humanitarian needs. • Protracted violence will force people to flee from their homes, deny them access to enough food, and rob them of their means of making a living. • Droughts, floods, hurricanes and other natural disasters will also create humanitarian needs. Although the risk of El Niño or La Niña is low next year, some scientists forecast an increased risk of earthquakes in 2018. • In a number of countries, humanitarian needs will fall, but still remain significant, including Afghanistan, Ethiopia, Iraq, Mali, and Ukraine. • However, needs are rising substantially in Burundi, Cameroon, Central African Republic, the Democratic Republic of the Congo, Libya, Somalia and Sudan. • And needs will remain at exceptionally high levels in Nigeria, South Sudan, the Syria region, and Yemen, which is likely to remain the world’s worst humanitarian crisis. • Overall, 136 million people across the world will need humanitarian assistance and protection. • UN-coordinated response plans costed at $22.5 billion can help 91 million. • The overall number of people in need is more than 5% higher than in the 2017 GHO. The cost of the response plans sets a new record, about 1% higher than at the start of 2017. • Humanitarian agencies will become more effective, efficient and cost-effective. They will respond faster to crises, in a way more attuned to the needs of those they are trying to help. They will undertake more comprehensive, cross-sectoral and impartial needs assessments. They will also contribute more to long-term solutions by working more closely with development agencies. • Larger country-based pooled funds will improve the agility and prioritised use of funds in the places where they operate. An expanded Central Emergency Response Fund will better support the least-funded major crises.
PEOPLE IN NEED PEOPLE TO RECEIVE AID 135.7M 90.9M
FINANCIAL REQUIREMENTS $22.5B
Sixteen men and three women have been arrested for allegedly aiding and abetting female genital mutilation (FGM) in eastern Uganda after reports of gangs attacking women in the region.
Wednesday, January 30th, 2019https://www.youtube.com/watch?v=_kmV61HgJCE
1/22/1979: 16-year old Brenda Spencer kills 2 men and wounds 9 children as they enter the Grover Cleveland Elementary School in San Diego.
Tuesday, January 29th, 2019“……currently serving a term of 25 years to life at the California Institution for Women in Corona, California. She has been denied parole four times, most recently in 2005…..”
https://www.youtube.com/watch?v=KXlhlztJRQc
1/22/1922: Accumulated snow on the Knickerbocker’s roof collapsed the building and tons of steel and concrete fell down on top of the theatergoers killing 108 and hospitalizing another 133.
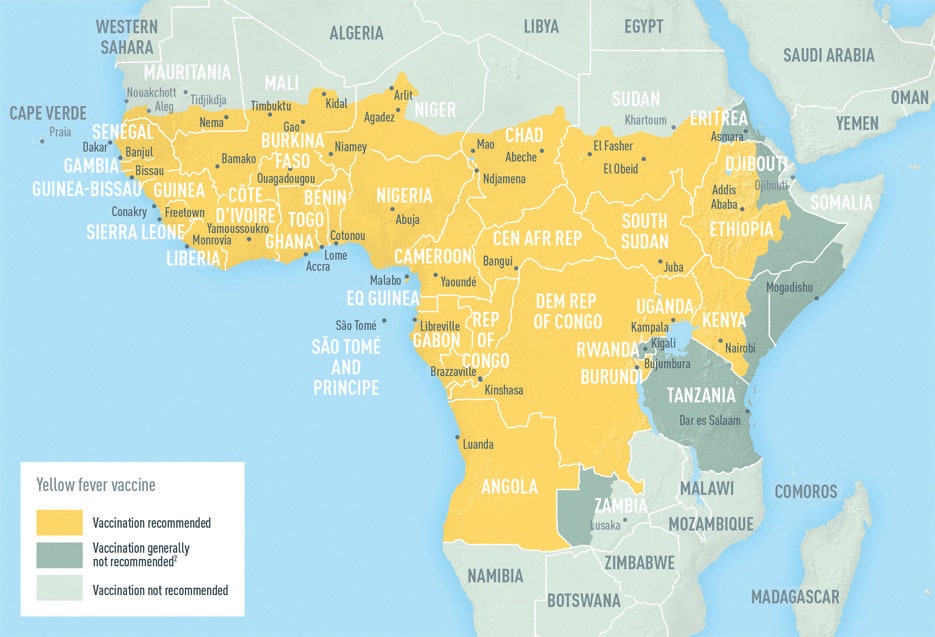
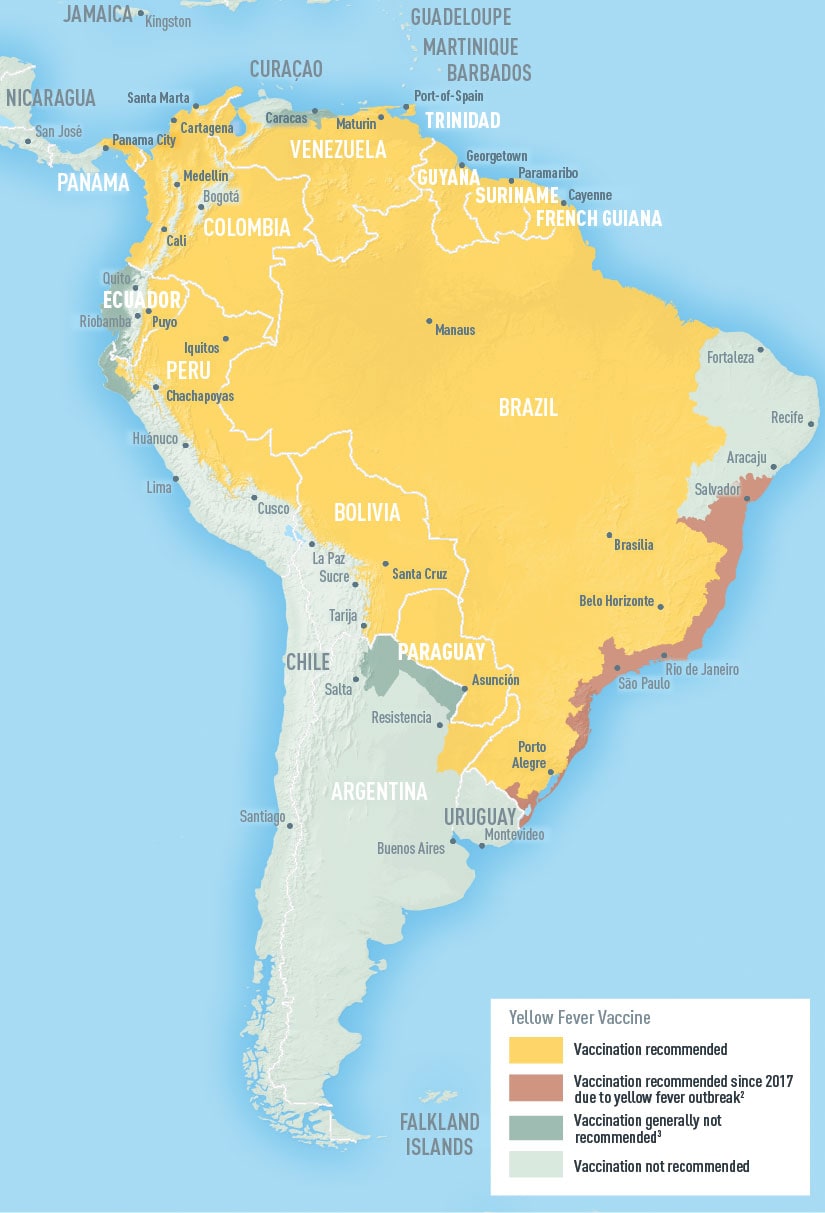
Tuesday, January 29th, 2019PAHO reported 12 new cases of yellow fever in Brazil, possibly marking the beginning of the country’s third wave of yellow fever activity in the past 2 years.
Tuesday, January 29th, 2019“…….In the 2016-17 yellow fever transmission cycle, Brazil saw 778 yellow fever cases, including 262 deaths. In 2017-18, that number grew to 1,376 cases, including 483 deaths, as the disease spread to regions with low vaccination rates...….”