Archive for the ‘Flood’ Category
NASA: After Hurricane Laura made landfall
Monday, August 31st, 2020August 13, 2020
August 29, 2020
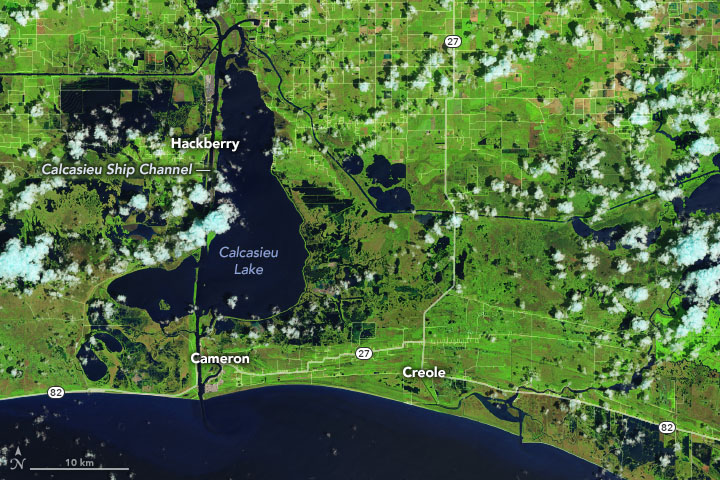
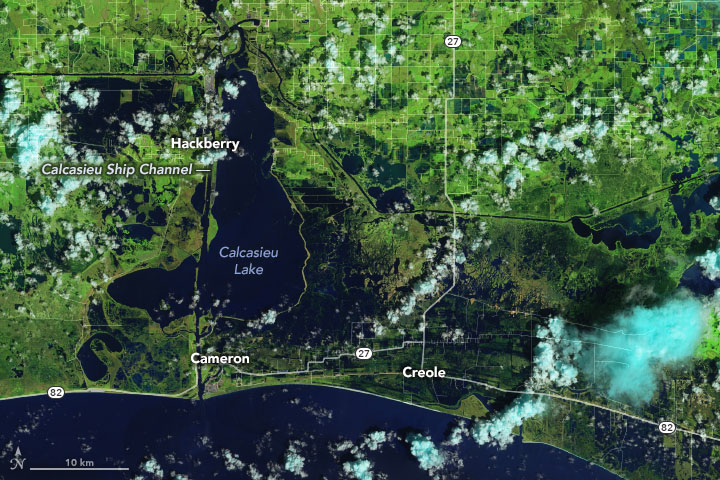
Hurricane Laura made landfall along the Louisiana and Texas coasts on August 26, 2020. In the wake of the category 4 storm, the Operational Land Imager (OLI) on Landsat 8 acquired images showing flooded coastal lands around the towns of Cameron and Creole, Louisiana, south of the city of Lake Charles. The false-color images were acquired on August 13 and 29, 2020. They were composed from a combination of shortwave infrared, near infrared, and natural color (bands 6-5-4) to make it easier to distinguish flooded areas (navy blue and black) from drier ground. Vegetation is bright green and clouds are cyan.
NASA Earth Observatory images by Joshua Stevens, using Landsat data from the U.S. Geological Survey and road data from OpenStreetMap. Caption by Michael Carlowicz.